Holiday Blues
- Kasie Marek

- Dec 11, 2019
- 7 min read
Processing... many of our days are spent processing.
Processing the events that have happened these last couple of weeks. After the last post and the hell of a 3 weeks Noah had, we needed time to just, process.

Many will never understand what this is like unless you've lived it. Like truly lived it; 24/7, watching your helpless baby struggle, seeing them "dissected" (as the doctors say), with an open chest and their organs right there in front of you. Only a few will really understand this journey, and get what we have seen these last 95 days.. the sounds we have heard, the lives lost we have witnessed in innocent babies. It's enough to knock you down. Make you question everything.
These last few months... we have changed.

Sure we are stronger, we love harder, but we are tired. We are depleted by the constant ups and downs. When we are certain things are headed in a good direction, we get slammed back down to the ground. Our bodies and hearts physically hurt watching Noah endure this.
We have had waves of emotions; PTSD, anger, fear, and anxiety.

There were multiple nights we were uncertain if we'd ever see Noah again. Sitting in the corner of the room, feeling helpless. As Noah's body turned blueish-grey, while the monitors alarmed and nurses moved rapidly around him. Going into cardiac arrest, the team having to do compressions on him...
It felt as if we were stuck in a bad dream, an out of body experience, a feeling that I wish upon no one.
Replaying those moments in our head multiple times throughout the day- and we've been struggling.
Brandon was supposed to be on a flight when the doctor came up to us and said: "your son might not make it"...

What if he wasn't there and something happened? Will we ever be able to leave the hospital for a split second without questioning if something will happen or go wrong?
Rewind to a couple of weeks ago when we first talked with the Heart Transplant team, I went into full-blown panic mode, crying uncontrollably.. the scary things that come with a transplant was a part of a whole new world that was foreign to us.

We have accepted that Noah would need the 3 surgeries for HLHS... so can't we just keep to that plan? We are angry. How was it that a couple of weeks ago we were home, and now we are back in the ICU with little hope that he can go home with his own heart.
As I sat in the family room that morning at 430 AM, crying.. pacing... praying..waiting to hear if Noah was alive. I asked God to give us more time. Whatever that meant. I begged for it. If we need to go transplant route, or if we need to go another route.... WHATEVER it meant... we will do it, just please give us more time.

And He delivered.
Since then, every time we hear heart transplant, it's just different; it means hope, it means more time.
Whether is a year or two, or twenty.
We have changed. We went into true war mode. We were ready to fight, and there were some institutional things that we weren't happy about. After processing the last traumatic night.. we needed to express that there were things that didn't seem right.

I won't go into detail, because I love so many people here, and we are forever grateful for the surgeon and doctors that have given us 4 amazing months with Noah.
But some things ruffled our feathers, and it was unacceptable. Since then, we have been working with the team to find solutions and I am thankful that at a chief level, they have taken the time to sit down and just listen to our concerns.

Lately the days have been long. Brandon and I have always been present for Noah- but when he is not well, we need to be 120 % present. And sometimes that means not taking calls, not posting updates, not eating.. or showering (gross I know).. but we have to. He needs us to advocate for him.
Seeing Noah intubated again was tough, he hated it. We had to keep him very sedated. He was extubated again 3 days later. His milrinone has increased to .75 (a pretty high dose) which is supporting his heart right now. Remember, this is the drug that is only IV, so if he does not tolerate coming off of this, then it means he will need a transplant- we can't live in the ICU forever..
After he started waking up from sedation after extubation, he was inconsolable. We were unsure if this was due to withdrawals from sedation or pain. That night I noticed that his pee was very smelly, I asked for a urine analysis which they did but didn't show infection.

For days, 4 days straight. Noah cried and wouldn't sleep for more than 15 minutes at a time, both day and night. It was terrifying. I would stare at him, trying to figure out what could be wrong. We ran every test on him, X-ray, ultrasound... everything!
It was extremely sad and frustrating to watch. Not knowing if he was hurting or something was wrong, it could have been anything- a scratch on his eye...his PICC line hurting, the possibility of things go on and on.
The team started to talk to us with their concerns that maybe it was neurological since there were times he didn't have oxygen to the brain and the last few very traumatic events on his body. The next day (Thanksgiving) as I watched him fall asleep, and as the little line on his diaper turned blue...he woke up from a sleep whimpering in pain... I thought it was something that was hurting him "down there". Luckily the nurse was attentive and expressed her concern to the team and another urine analysis was ordered, sure enough... a terrrrible UTI which came back from the culture as E.Coli, thankfully it didn't go any further since he had it for more than 5 days at that point. I felt terrible that he had been hurting so much and even with morphine it didn't help the pain but I was relieved that it was "just a UTI".

Antibiotics were started and Noah began to slowly feel better and get more rest. During this time we were also weaning him from Dex and multiple other drugs like ativan, morphine, etc.
Dex has never reacted well with him though and weaning from it sucks, but we were ready to get him off of it fast.
Then his heart rate struggled and he started vomiting...a lot. A baby's heart rate should be 120-160.. but the slower his heart rate, the less it is having to pump and work, so ideally we would want it around 130s awake! Noah was sleeping and his heart rate would be in the 180s with very hard breathing. Doctors adjusted some medications, and in the last week it has come down very nicely. It was terrifying seeing his heart rate at nearly 200 while he was calm. He received a couple blood transfusions which made him feel a little better.

The doctors then determined that his diaphragm was paralyzed; a complication that can happen during open-heart surgery which can make it difficult for Noah to breath causing him to rely on oxygen.
can. he. catch. a. break.

In many cases, surgery is needed to fix the diagram but with a little O2 support and extra time to heal, plus physical therapy doing some amazing work with him, we successfully pulled Noah off oxygen yesterday. It sounds so silly, but seeing his bare cheek (no tape or cannula) meant the world to me, I kissed it so many times.
Right now we are still working on his vomiting issue. this can be caused for a lot of reasons, and not tolerating feeds can be a sign of heart failure, but we are hopeful that this is not the case since he was taking feeds fine before.

He will not take a bottle at all. Oral aversions are common in these babies since they have a lot of negative experiences with things being in their mouth and the recent intubation was through Noah's mouth since it was an emergency. We have also (due to the vomiting) had to place him on continuous feeds last week, meaning he is getting fed all the time (via NG tube through the nose) a very small amount so it is easy on the stomach. We additionally switched him to a "broken down" formula that is easier on his tummy, and let's just say it smells disgusting so I am sure it doesn't taste any better.

Since he is getting continuous feeds, he is never hungry- every bottle attempt he has been uninterested.
Things have started to look up the last couple of days, but we know too well how fast things can change.
So we are soaking up all the smiles and sweet sounds!
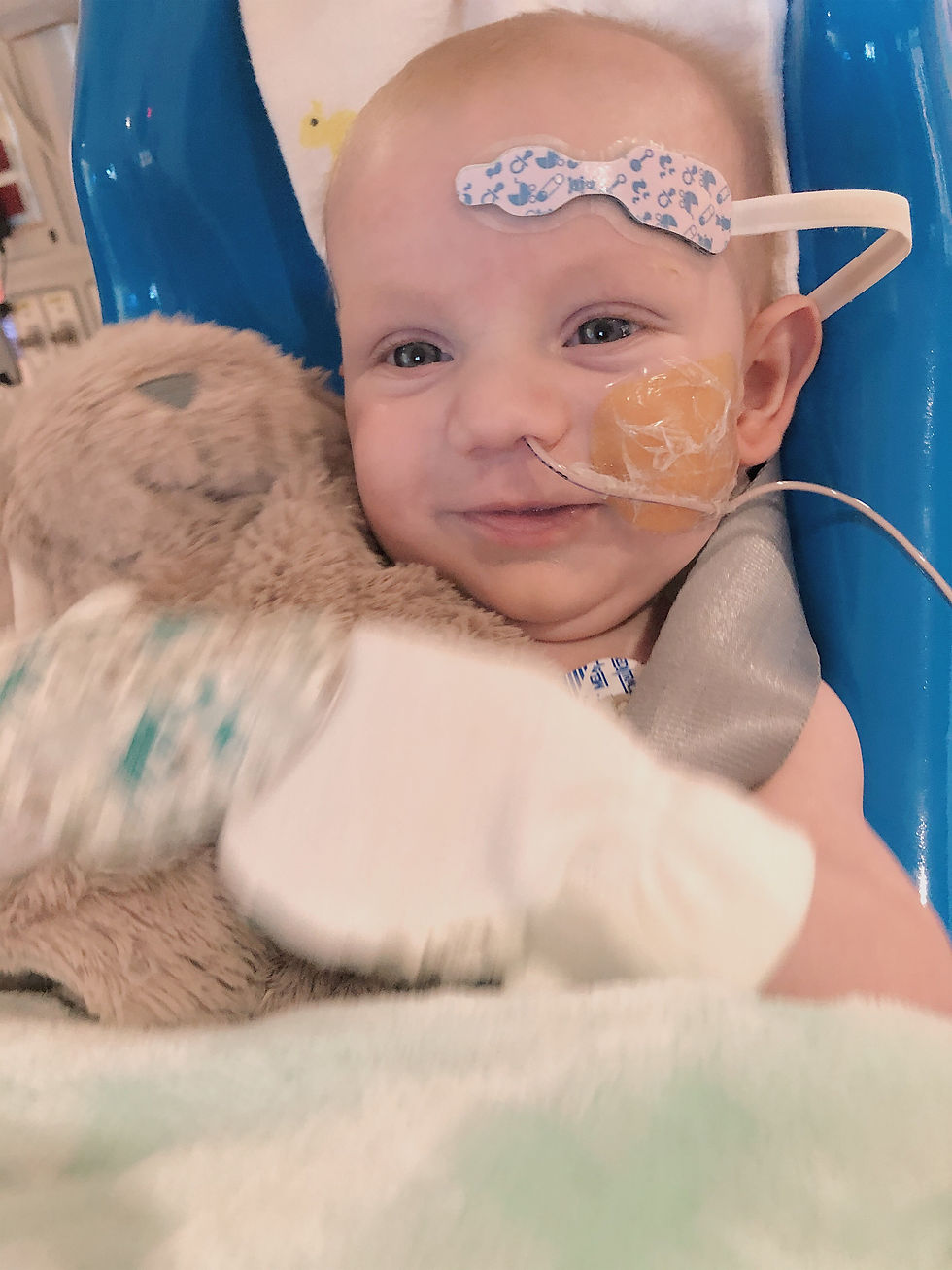
Next steps? Wean the milrinone and get him taking full feeds by mouth and tolerating them!
Last week we attempted to wean the milrinone from .75 to .5 and it didn't go well. He started getting very irritable and his heart rate shot back up with heavy breathing, NIRs dropping, ultimately increasing back to .75 in the middle of the night.

Friday will be the next attempt to start the wean and this will be a huge determining factor on if the home is on the horizon anytime soon.
We are actively working on feeds daily with Occupational Therapy, but we have a long way to go.

Each day is filled with many changes- lots of ups and downs- new goals- setbacks... all...the...things. And it can be difficult for friends and family to know what to do or say.
Many messages that we receive go unanswered because we can't keep reliving our days over and over and trying to explain things- we are tired but we are thankful you care and are invested in Noah's story. I will try to do a better job at posting daily, even if short updates.

We do not want our friends and family to be shied away because they don't know what to say. There is nothing you can say to make this better and honestly we want to just have NORMAL conversations that aren't consumed with heart stuff. Tell us about your day.. tell us a funny story.. We talk medical banter all day with the doctors and yes sometimes we just want to not think about it for a split second.

I apologize for the lengthy, all over the place, long-overdue post! Please continue to keep Noah in your thoughts and pray that we can successfully wean him off Milrinone!



NOAH has the most gorgeous blue eyes.and that smile.will take your breath away.He will always be in my prayers.and I do PRAY you Mom and Dad.God will bless y'all .I have actually let my heart open and put you three in there.y'all will always have a special part of my heart..#team NOAH.